How do beta lactamases degrade beta lactams
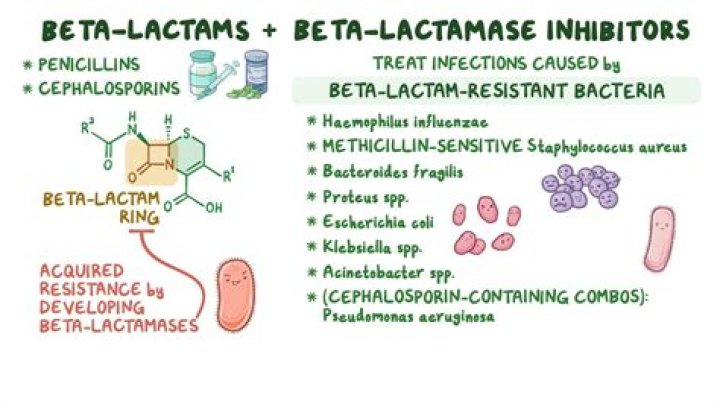
In a second step, nucleophilic attack by a water molecule cleaves the covalent bond between the enzyme and the carbonyl group of the erstwhile beta-lactam. This allows the degraded beta-lactam to diffuse away and frees up the enzyme to process additional beta-lactam molecules.
Do beta-lactamases break the beta-lactam ring?
Beta-lactamases are enzymes produced by bacteria that break open the beta-lactam ring, inactivating the beta-lactam antibiotic. Some beta-lactamases are encoded on mobile genetic elements (eg, plasmids); others are encoded on chromosomes.
How are beta lactams eliminated?
Beta-lactam antibiotics are hydrophilic molecules and most beta-lactams are eliminated primarily through the kidneys, making their pharmacokinetics (PK) highly susceptible to alterations seen in critical illness.
How does beta-lactamase destroy penicillin?
The beta-lactam ring is essential for penicillin’s activity. Bacteria that can destroy penicillin do so by secreting enzymes called beta-lactamases. These enzymes cleave the beta-lactam ring of penicillin so that the drug becomes inactive.What do beta-lactamases do?
The beta-lactamase enzymes inactivate beta-lactam antibiotics by hydrolyzing the peptide bond of the characteristic four-membered beta-lactam ring rendering the antibiotic ineffective. The inactivation of the antibiotic provides resistance to the bacterium.
How do β lactams affect and destroy bacteria?
The β-lactams are bactericidal agents that kill bacteria by interrupting peptidoglycan (cell wall) biosynthesis. Their targets are penicillin-binding proteins (PBPs) that exhibit transglycosylase/transpeptidase or carboxypeptidase activities in both Gram-positive and Gram-negative bacteria.
Does beta-lactamase degrade ampicillin?
The satellites form because the beta-lactamase released by the bla-expressing colony degrades the ampicillin in the vicinity of the colony. The satellites are not necessarily a problem as they will not grow when transferred to a medium containing fresh ampicillin.
How does penicillin inhibit Transpeptidase?
Penicillin irreversibly inhibits the enzyme transpeptidase by reacting with a serine residue in the transpeptidase. This reaction is irreversible and so the growth of the bacterial cell wall is inhibited.What is penicillin ineffective against?
Penicillin is effective only against Gram-positive bacteria because Gram negative bacteria have a lipopolysaccharide and protein layer that surrounds the peptidoglygan layer of the cell wall, preventing penicillin from attacking.
How does penicillin inhibit cell wall synthesis?Penicillin kills bacteria through binding of the beta-lactam ring to DD-transpeptidase, inhibiting its cross-linking activity and preventing new cell wall formation. Without a cell wall, a bacterial cell is vulnerable to outside water and molecular pressures, which causes the cell to quickly die.
Article first time published onIs penicillin bacteriostatic or bactericidal?
Penicillins are bactericidal beta-lactam antibiotics that inhibit bacterial cell wall synthesis. A natural product, the penicillin structure has been modified to prepare a variety of semi-synthetic agents.
Are all penicillins beta lactams?
Beta-lactam antibiotics include penicillins, cephalosporins and related compounds. As a group, these drugs are active against many gram-positive, gram-negative and anaerobic organisms.
Can b lactamase degrade vancomycin?
β-lactamases can degrade vancomycin. 24 . Echinocandins, known as “penicillin for fungi,” target β(1→3) glucan in fungal cell walls.
How does beta lactamase produce resistance against penicillin?
The most common mechanism of β-lactam resistance among bacteria is the production of a β-lactamase, which is an enzyme that cleaves the key structure of the antimicrobial agent, that is, the β-lactam ring. This renders the drug inactive.
Are cephalosporins beta-lactamase resistant?
Some species of bacteria produce beta-lactamase enzymes, which cleave the beta-lactam group in antibiotics, such as cephalosporins, that have a beta-lactam ring in their structure. In doing so the beta-lactamase enzyme inactivates the antibiotic and becomes resistant to that antibiotic.
Which penicillin is resistant to beta-lactamase?
DrugTargetTypeOxacillinPenicillin-binding protein 2atargetOxacillinPenicillin-binding protein 1AtargetOxacillinPenicillin-binding protein 2BtargetOxacillinPenicillin-binding protein 1btarget
Does beta-lactamase produced by bacteria affect amoxicillin or ampicillin?
For example, Augmentin (FGP) is made of amoxicillin (a β-lactam antibiotic) and clavulanic acid (a β-lactamase inhibitor). The clavulanic acid is designed to overwhelm all β-lactamase enzymes, and effectively serve as an antagonist so that the amoxicillin is not affected by the β-lactamase enzymes.
How does tetracyclines antibiotics affect and destroy bacteria?
Tetracycline interferes with the ability of the bacteria to produce certain vital proteins required for bacterial growth. They target the ribosomal machinery within the bacteria that assembles proteins from amino acids. Due to this mode of action, tetracyclines inhibit bacterial growth rather than killing them.
How do tetracyclines affect and destroy bacteria?
Tetracyclines probably penetrate bacterial cells by passive diffusion and inhibit bacterial growth by interfering with protein synthesis or by destroying the membrane. A growing number of various bacterial species acquire resistance to the bacteriostatic activity of tetracycline.
Are beta lactams bactericidal or bacteriostatic?
β-Lactam antibiotics are bactericidal agents that interrupt bacterial cell-wall formation as a result of covalent binding to essential penicillin-binding proteins (PBPs), enzymes that are involved in the terminal steps of peptidoglycan cross-linking in both Gram-negative and Gram-positive bacteria.
How do bacteria become resistant to antibiotics?
There are two main ways that bacterial cells can acquire antibiotic resistance. One is through mutations that occur in the DNA of the cell during replication. The other way that bacteria acquire resistance is through horizontal gene transfer.
How does misuse of antibiotics lead to resistance?
Anytime antibiotics are used, they can contribute to antibiotic resistance. This is because increases in antibiotic resistance are driven by a combination of germs exposed to antibiotics, and the spread of those germs and their mechanisms of resistance.
Which of the following is resistant to penicillin?
Bacteria resistant to antibiotics For example, Staphylococcus aureus (‘golden staph’ or MRSA) and Neisseria gonorrhoeae (the cause of gonorrhoea) are now almost always resistant to benzyl penicillin. In the past, these infections were usually controlled by penicillin.
Does penicillin bind to transpeptidase?
Penicillin-binding protein, transpeptidaseIdentifiersOPM protein5hlbMembranome541showAvailable protein structures:
Where do macrolides exhibit their mechanism of action?
Mechanism of action Macrolide antibiotics do so by binding reversibly to the P site on the 50S subunit of the bacterial ribosome. This action is considered to be bacteriostatic. Macrolides are actively concentrated within leukocytes, and thus are transported into the site of infection.
Which among the following inhibits the transpeptidase activity?
The antibiotic penicillin irreversibly binds to and inhibits the activity of the transpeptidase enzyme by forming a highly stable penicilloyl-enzyme intermediate. Because of the interaction between penicillin and transpeptidase, this enzyme is also known as penicillin-binding protein (PBP).
How does beta lactam inhibit cell wall synthesis?
β-Lactam antibiotics inhibit bacteria by binding covalently to PBPs in the cytoplasmic membrane. These target proteins catalyze the synthesis of the peptidoglycan that forms the cell wall of bacteria. Alterations of PBPs can lead to β-lactam antibiotic resistance.
What part of the cell does penicillin inhibit?
Penicillin interferes with the production of a molecule called peptidoglycan. Peptidoglycan molecules form strong links that give the bacterial cell strength as well as preventing leakage from the cytoplasm. Nearly every bacterium has a peptidoglycan cell wall.
Which of the following antibiotics would inhibit cell wall synthesis?
Penicillins and cephalosporins are the major antibiotics that inhibit bacterial cell wall synthesis.
Which drug is bactericidal?
Bactericidal antibiotics that inhibit cell wall synthesis: the beta-lactam antibiotics (penicillin derivatives (penams), cephalosporins (cephems), monobactams, and carbapenems) and vancomycin. Also bactericidal are daptomycin, fluoroquinolones, metronidazole, nitrofurantoin, co-trimoxazole, telithromycin.
How do bactericidal antibiotics work?
Some antibacterials (eg, penicillin, cephalosporin) kill bacteria outright and are called bactericidal. They may directly attack the bacterial cell wall, which injures the cell. The bacteria can no longer attack the body, preventing these cells from doing any further damage within the body.